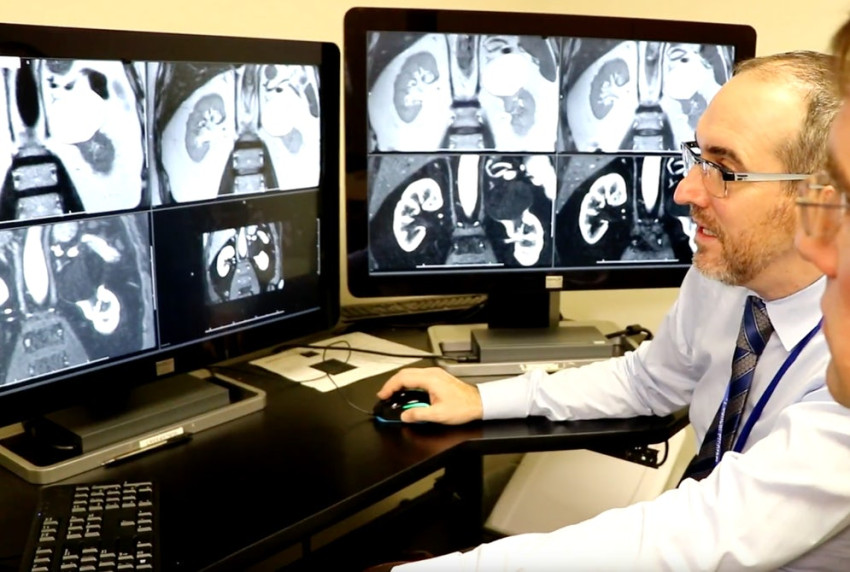
New approach to MRI scans replaces biopsies
A new combination of MRI scans clarifies directly whether a kidney tumour is benign or malignant. This may reduce the number of biopsies, avoiding having to remove tumour tissue for examination. The technique has been developed by doctors and engineers in a cancer hospital in Texas.
Kidney tumours are often discovered by accident. While carrying out a scan for other medical reasons, the kidney shows a lump of tissue that shouldn't be there.
If a doctor discovers such a lump, then he or she carries out a follow-up examination to determine what type of tumour it is. If the tissue is benign, then it is usually left alone. But an aggressive, malignant tumour needs to be treated as quickly as possible.
Needle

tissue.
For this follow-up examination, the doctor usually removes a small amount of tissue from the tumour with a biopsy. The pathologist then examines this tissue in the laboratory. During a biopsy, the doctor inserts a needle into the kidney and uses that needle to remove a small amount of tissue. This causes discomfort or pain for the patient, and is also not without risk: each intervention brings with it an additional risk of infection, for example.
New MRI protocol
So it would be great if doctors could learn more about the tumour without having to resort to such invasive surgery. It looks like this could now become a reality. Doctors and engineers from the UT Southwestern Harold C. Simmons Comprehensive Cancer Center in the United States have developed a new MRI protocol that determines with a high degree of reliability whether a tumour is benign or not.
‘We generate various different pictures of the kidney, and these tell us something about the tissue’, explains Professor of Radiology Ivan Pedrosa, one of the inventors of the technique in a press release. This new method combines different ways of carrying out an MRI scan. Firstly ‘standard’ images are generated. Then scans are carried out of the kidney after a contrast liquid is injected into the bloodstream. A third type of scan shows whether there is any fatty tissue in the tumour. By playing with the settings of an MRI scanner, images of certain types of tissue can be generated as required, while others remains dark (see for instance the table in this explanation of an MRI).
Recognizing cancer
An algorithm is then employed using all the useful information that can be retrieved from these images. The technique is called ‘multi-parametric MRI’. The algorithm indicates to a confidence level of some 80% whether or not the lump of tissue is clear-cell kidney cancer (this aggressive variant of kidney cancer is by far the most common type, representing 70 to 80% of all cases). This means that doctors have a four-out-of-five chance of recognizing this type of kidney cancer using the new MRI method. That is still far too low to provide a reliable diagnosis, so the confidence level will have to be increased. However, multi-parametric MRI can already play a supporting role.
Fewer biopsies needed
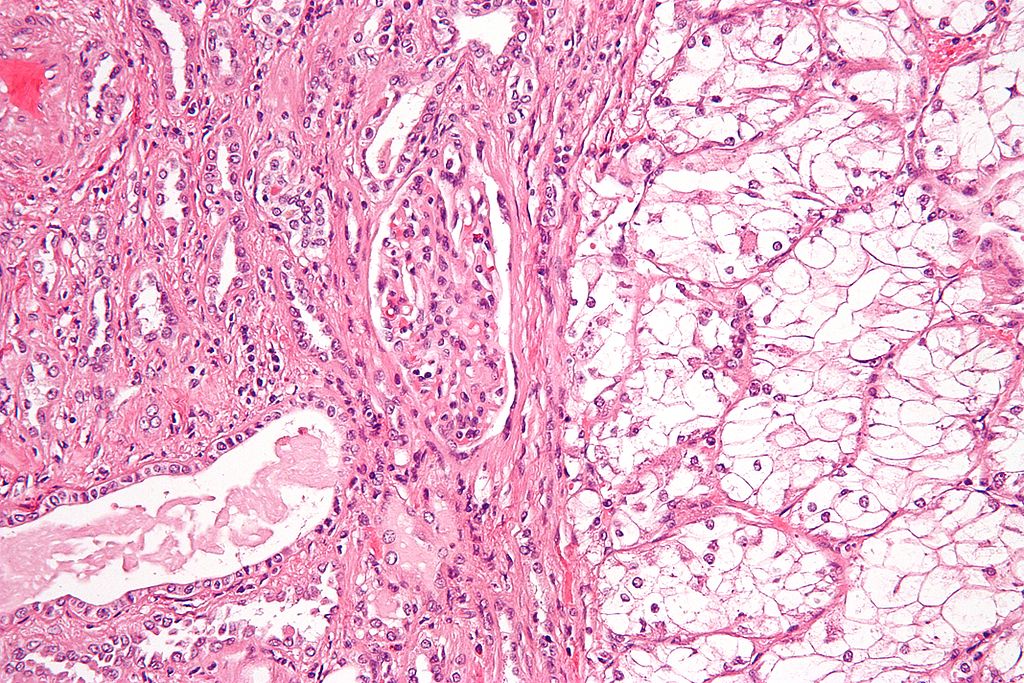
slices that are coloured with a dye to better indicate
certain cell types. Here you can see a microscopic
image of such a slice that allows the pathologist
to look for cancer cells. In this case, it's the white
area to the right of the tumour. Photo Nephron
/ Wikimedia Commons
Eventually the new MRI method could mean that fewer biopsies are needed. ‘Biopsies are not entirely pain-free. Some patients even choose not to undergo a biopsy to avoid the pain’, said Jeffrey Cadeddu, Professor of Urology and Radiology in the same press release.
The researchers involved are continuing to develop their MRI technique, so that in future they can detect not only the nature of the tumour, but also ascertain how aggressive it is. After all, this information enables the doctor to partly gauge how best to treat the patient.
If you found this article interesting, subscribe for free to our weekly newsletter!
Opening image: radiologists Ivan Pedrosa and Jeffrey Cadeddu discuss a patient's MRI scans. Source UT Southwestern.
Meer artikelen

Een AI-fabriek in Groningen

Gezondheid meten via zweetdruppels
Nieuwste artikelen

Een AI-fabriek in Groningen






